Current Issue
Delayed Diagnosis of Twin-Twin Transfusion Syndrome in Humanitarian, Resource-Limited Settings: A Case Report
Jerom Okot1*, Henry Ochola2, Michael Job Aeku1, Nelson James Okema1, Felix Bongomin3, Simple Ouma4,5, Francis Pebalo Pebolo6
1Faculty of Medicine, Gulu University, Gulu, Uganda
2Faculty of Epidemiology and Population Health, London School Hygiene and Tropical Medicine, London, United Kingdom
3Department of Medical Microbiology, Faculty of Medicine, Gulu University, Uganda
4Department of Public Health, Gulu University, Uganda
5The AIDS Organization, Kampala, Uganda
6Department of Sexual and Reproductive Health, Gulu University, Uganda
*Corresponding author: Jerom Okot, Faculty of Medicine, Gulu University, Gulu, Uganda, Tel: +256769641285, E-mail: [email protected]
Citation: Okot J, et al. (2026). Delayed Diagnosis of Twin-Twin Transfusion Syndrome in Humanitarian, Resource-Limited Settings: A Case Report. Cases. 5(1):27.
Copyright: Okot J, et al. © (2026).
ABSTRACT
Background: Twin-to-twin transfusion syndrome, though rare, poses risks for fetal demise if undetected. This late-diagnosed Twin-Twin Transfusion Syndrome case from South Sudan demonstrates persistent challenges in identifying high-risk pregnancies in humanitarian settings. Case presentation: A 38-year-old multigravida at unknown weeks’ gestation presented with fever, labour pains, drainage of liquor, and fetal hand prolapse. Her antenatal care only reported non-specific symptoms without most diagnostics. Evaluation revealed malaria, suspected twin pregnancy, and malpresentation. Undiagnosed Twin-Twin Transfusion Syndrome became apparent only during emergent cesarean delivery, finding a demised anomalous donor twin. The acute intrapartum decompensation pointed to stage V Twin-Twin Transfusion Syndrome. Conclusion: This case reinforces literature on missed screening opportunities to recognize Twin-Twin Transfusion Syndrome before Quintero staging with poorer prognoses. Subtle signs like sudden abdominal enlargement during third trimester were likely overlooked due to limited access to comprehensive ultrasound and Doppler surveillance. Strengthening displacement-sensitive antenatal protocols, building frontline imaging capacity, improving provider awareness, and prompt referrals could help mitigate Twin-Twin Transfusion Syndrome -related morbidity and mortality in marginalized populations. Global health efforts must address these persisting care gaps in pregnancy surveillance and access to specialty care, especially in humanitarian settings.
Received Date: November 14, 2025 Publication Date: March 30, 2026
Keywords: Twin-Twin Transfusion Syndrome, Monochorionic Twins, Humanitarian Settings, Low-Resource Obstetrics, Prenatal Diagnosis, Northern Uganda
BACKGROUND
Twin-to-twin transfusion syndrome (TTTS) occurs in 10–15% of monochorionic twins and arises from arterial-venous anastomoses on the shared placenta, leading to unbalanced flow from one fetus (the "donor") to another (the "recipient") [1]. The pathophysiology arises from the incomplete division between the fetal circulations that creates vascular communications which lead to inadequately balanced blood flow and compensation between the foetuses [2]. The recipient twin progressively accumulates excess circulating volume in the setting of hyperdynamic cardiac function and downstream hemodynamic changes. Meanwhile, the donor twin experiences progressively diminished circulating volume resulting from persistent net transfer towards the recipient [3]. This results in oligohydramnios around the donor and polyhydramnios around the recipient, with twin discordance in size, weight and amniotic fluid. If left untreated, this imbalanced perfusion and transfusion ongoing in utero culminates in up to 70-100% mortality from heart failure, hydrops, entanglement of cords or preterm birth [1-3].
The reference standard for diagnosis remains comprehensive ultrasonography, characterizing features like oligo-/polyhydramnios sequence, “stuck” twin, and bladder signaling in addition to growth restriction or cardiac dysfunction [4]. Cardinal symptoms reported by pregnant women - such as sudden-onset abdominal swelling, pelvic pressure or dyspnea - may also alert providers [5]. Definitive treatment is fetoscopic laser coagulation to permanently ablate placental vascular communications [6]. This has led to improved survival of at least one twin in 56-100% of TTTS cases and reduced neurological morbidity compared to other invasive interventions like amnioreduction [6]. However, optimal outcomes rely on delivery at experienced, high-volume fetal therapy centers before potential losses or end-organ sequelae and access to specialized teams for treatment poses challenges globally, even in high-income countries [7,8].
In regions with few fetal therapy resources, few data exist on coupled detection-to-delivery trajectories in TTTS. This likely contributes towards preventable losses, where early surveillance and diagnosis could prompt life-saving referrals. Our case helps illustrate such pitfalls in marginalized health systems. Understanding where hidden prevalence may remain in displaced or low-resource populations could also spotlight needed interventions, whether through capacity-building, provider education or temporary surgical missions.
CASE PRESENTATION
A 38-year-old female, G11P10+1 at 36 weeks and 5 days of gestation by obstetric ultrasound scan, admitted at a rural Ugandan Health Center level IV in Lamwo District, Northern Uganda. She was received as a referral from a remote Health Centre II, a low-level health facility in neighboring South Sudan, due to arm prolapse in labour for further management.
History of Present Illness: The patient had a 5-day history of intermittent high-grade fever followed by a 3-day report of labour-like pain associated with per-vaginal drainage of clear, odorless fluid prior to referral. She reported feeling fetal kicks and denied per-vaginal bleeding, lower urinary tract symptoms, headache, nausea, or vomiting.
Antenatal History: She attended antenatal clinic 7 times at the referral site, was booked in the first trimester, screened sero-negative for syphilis and Human Immuno-deficiency Virus (HIV), and received ferrous sulphate, folate, tetanus-toxoid, mebendazole, and fansidar. She had normal blood pressures and normal abdominal palpation findings, but no serial fundal height measurements, urinalysis, or obstetric scan were performed. She had no other recurrent illness during this pregnancy. Pre-referral, no tests were done but the patient was pre-medicated with oral paracetamol.
Past Obstetric and Medical History: All her previous pregnancies were singleton, delivered vaginally; however, the last pregnancy was preterm at 28 weeks of gestation with neonatal death at 4 hours postpartum (cause of death unknown). She had no known chronic medical illness and reported a change of paternity since the preceding pregnancy following the death of her first spouse due to an unknown cause. She is a peasant who resides with her 9 offspring on a farm homestead in South Sudan and reported no further fertility desire.
Clinical Findings on Admission
On Examination, she was in pain with a self-reported pain scale of 7/10, had mild dehydration, and was febrile (38.6°C) but had no pallor or jaundice. She was normotensive (blood pressure: 120/75mmHg) with a normal pulse rate of 90 beats per minute.
The obstetric exam found a symphysial-fundal length of 37cm, cephalic fetal presentation, oblique lie, normal fetal heart rate (130 beats per minute), a descent of 5/5th palpable, and 1-2 uterine contractions in 10 minutes each lasting 10-20 seconds. A sterile speculum vaginal exam revealed odorless liquor with a positive pooling test, a fetal hand prolapsed into the vagina, and cervical dilation of 3cm with no cord prolapse.
Investigations
Initial laboratory tests were positive for malaria via rapid diagnostic test. Full blood count showed mild leukocytosis (12x10?/L), thrombocytopenia (92x10?/L), and a normal hemoglobin level (13.3g/dl). Blood group was A rhesus positive and urine dipstick was normal.
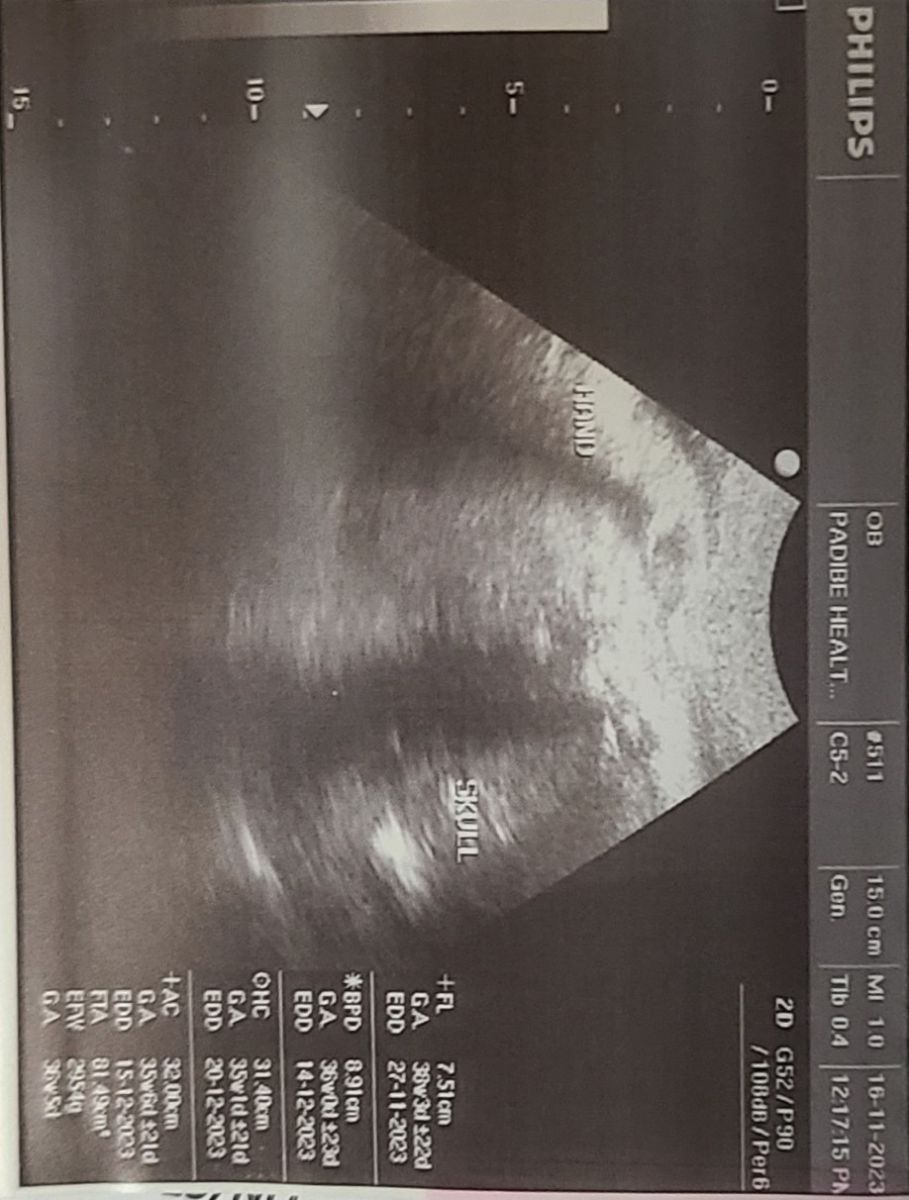
An obstetric scan done revealed a single live fetus at 36 weeks and 5 days of gestation, estimated weight of 2954 grams, mild polyhydramnios, compound presentation, (Figure 1).
Figure 1: Ultrasound scan image
At this point, the admission diagnosis was latent labour with preterm pre-labor rupture of membranes, compound presentation with hand prolapse, and severe malaria with mild thrombocytopenia.
Management
On the day of admission, she was started on intravenous (IV) artesunate 127mg at 0, 12, and 24 hours followed by oral (po) artemether-lumefantrine (80/480mg) 12 hourly for 3 days, po paracetamol 1g 8 hourly for 3 days, and IV ceftriaxone 1gm once daily for 5 days.
The patient was counselled for an emergency caesarean section due to the compound presentation with hand prolapse and for concurrent bilateral tubal ligation. Informed consent was obtained, blood was cross-matched, and the patient was preloaded with 1 liter of IV normal saline.
The caesarean section was performed under spinal anesthesia via a Pfannenstiel incision. An intact gravid uterus was found. A lower uterine segment incision was made, delivering a live baby boy (Twin A), weight 2500 grams, with APGAR scores of 8 and 10 at 1 and 5 minutes, respectively. A second macerated, compressed fetus (Twin B) of indistinguishable sex, weighing 200g, was delivered from the left aspect of the uterus. A single monochorionic diamniotic placenta was delivered by controlled cord traction. The umbilical cords were separate and inserted normally. The uterus was closed in layers. Bilateral tubal ligation was performed using the Parkland technique. The estimated blood loss was 400 milliliters.
Postoperative Course & Placental Findings
Postoperatively, the patient received maintenance IV fluids, analgesics, IV metronidazole, and continued the drugs prescribed on admission. The newborn commenced breastfeeding and was well.
Placental examination confirmed a single disc with diamniotic membranes and two separate umbilical cords (two-vessel cords each). Vascular anastomoses on the chorionic plate were noted but not mapped in detail.
Neonatal evaluation of the surviving twin was limited by facility resources; the baby was clinically well with stable vitals and a normal physical exam. Advanced assessments (echocardiogram, cranial ultrasound, hematocrit differential) were not available.
Both mother and baby were discharged in good condition on the third postoperative day.
DISCUSSION
This case illustrates key challenges surrounding diagnosis and management of TTTS in low-resource settings. The subtle signs of TTTS were likely missed during routine antenatal care for this patient from South Sudan, ultimately leading to an adverse outcome.
While the classic features were eventually noted such as polyhydramnios, and growth discordance earlier detection of the twin pregnancy may have been possible with risk-based screening incorporating first trimester ultrasound and Doppler studies as availability allowed [9]. However, the remote setting and displaced status of this patient hindered access to such diagnostics, a recognized barrier in similar humanitarian contexts. Consequently, progression to more severe Quintero staging could not be halted pharmacologically or through laser intervention [1].
Undiagnosed TTTS also posed delivery challenges once unrecognized severe growth discrepancy and malpresentation came to light. Accessing emergency cesarean capabilities in such a remote setting averted likely adverse outcomes for the second twin but this may not be feasible for all patients [10].
Notably, this case adds to limited literature on TTTS in displaced or low-resource populations. While successful introduction of laser surgery has been demonstrated elsewhere, preventing late diagnoses remains paramount [10]. This reinforces the value of raising TTTS awareness and building frontline ultrasound capabilities for earlier detection where possible . More population data on TTTS-attributable morbidity could also strengthen the impetus for such health systems strengthening.
In low-income regions, complex fetal disorders like TTTS continue posing diagnostic and therapeutic challenges. As illustrated through this case, opportunities exist for quality improvement through risk-appropriate antenatal screening, telehealth support of providers, patient education and enhanced surgical capacity-building. Reporting this experience from South Sudan thus highlights where global health resources could be focused to improve care for vulnerable women and babies.
A critical missed opportunity was the absence of any obstetric ultrasound during ANC. While first-trimester scanning is ideal, a single second-trimester scan to establish chronicity would have identified this as a high-risk monochorionic pregnancy. Without this, serial monitoring for early TTTS signs (discordant amniotic fluid or growth) was impossible. This case underscores a common system failure in low-resource ANC: an over-reliance on basic palpation and medication distribution, while omitting fundamental risk-assessment tools. Even simple interventions, like serial symphysis-fundal height measurement, may have signaled polyhydramnios or rapid uterine growth suggestive of a multiple pregnancy. The remote, humanitarian context of this patient from South Sudan presents a unique barrier, limiting access to diagnostics and specialized care. This directly mirrors outcomes in similar settings where TTTS is typically diagnosed only after irreversible progression, often at delivery. The emergent compound presentation and hand prolapse were direct consequences of the undiagnosed polyhydramnios, transforming the delivery into a surgical emergency. While accessing a cesarean section averted a double fatality, it represents a crisis response rather than planned management.
CONCLUSION
This case report presents a late-diagnosed and undiagnosed TTTS in a low-resource humanitarian setting, resulting in demise of the donor twin. The subtle signs pointing to TTTS during pregnancy were likely overlooked due to limitations in diagnostic capacity and prenatal screening protocols in the region. While the surviving twin was ultimately delivered via emergency cesarean, earlier detection could have allowed for specialist referral, fetal intervention, and possible prevention of a demise.
Key clinical takeaways highlight persistent gaps in identifying high-risk pregnancies in displaced or low-resource populations, leading to missed opportunities for mitigating morbidity and mortality from conditions like TTTS. Strengthening frontline screening with ultrasound, improving provider knowledge, and enhancing coordination for referrals and transport are imperative to pick up danger signs earlier. smoothly. More widespread data on TTTS-attributable adverse outcomes could also inform health policy and resource allocation in vulnerable settings.
This case stresses the importance of investing in healthcare infrastructure and delivery systems serving pregnant women in low-income regions. Reporting experiences such as this brings awareness to where global health efforts must be focused to advance maternal-fetal medicine in areas struggling with access barriers. Knowledge-sharing around successful introduction of specialized capabilities like foetoscopic surgery elsewhere provides hope for incrementally tackling complex conditions like TTTS at the margins of the healthcare system.
ACKNOWLEDGEMENT
We acknowledge medical students from Gulu University and Padibe Health Centre IV.
STATEMENTS
Conflict of Interest
The authors declare that they have no conflict of interest.
Data Availability Declaration
Data on the history and management of the mother and baby are available upon reasonable request from the first Author
Ethic Approval and Consent to Participate
The mother provided written informed consent for the case to be published,
REFERENCES
- Abgral M, Dumery G, Mégier C, Leyne E, Luton D, Benachi A, et al. (2025). Twin-to-twin transfusion syndrome: from pathophysiology to long-term outcome-a narrative review. European Journal of Pediatrics. Dec;185(1):24.
- Finnemore A, Groves A. (2015). Physiology of the fetal and transitional circulation. Seminars in Fetal & Neonatal Medicine. 20(4):210-216.
- Jian W, Guo D, Yao R, Pei M, Guo M, Yang F. (2025). Cardiac function impairment in recipient twins of twin-to-twin transfusion syndrome: Insights from NT-proBNP levels in amniotic fluid. Clinical Biochemistry. 136:110894.
- Durbin SA. (2011). A Sonographer’s Perspective: Quintero Staging System for Twin-to-Twin Transfusion Syndrome in Monochorionic Twins. Journal of Diagnostic Medical Sonography. 27(3):122–125.
- Ertmann RK, Nicolaisdottir DR, Kragstrup J, Overbeck G, Kriegbaum M, Siersma V. (2023). The predictive value of common symptoms in early pregnancy for complications later in pregnancy and at birth. acta obstetricia et gynecologica scandinavica. 102(1):33–42.
- Javinani A, Oyelese Y, Chervenak FA, Grünebaum A, Chmait RH, Papanna R, et al. (2024). Fetoscopic laser photocoagulation: a medically reasonable treatment option in the management of types II and III vasa previa. Journal of Perinatal Medicine. 26;52(9):927–933.
- Bouchghoul H, Madar H, Mattuizzi A, Coatleven F, Vincienne M, Prier P, et al. (2025). Management of twin?to?twin transfusion syndrome: update and current challenges. American journal of obstetrics & gynecology MFM. 7(8):101714.
- Spruijt MS, Lopriore E, J. Steggerda S, Slaghekke F, Van Klink JMM. (2020). Twin-twin transfusion syndrome in the era of fetoscopic laser surgery: antenatal management, neonatal outcome and beyond. Expert review of hematology. 13(3):259–267.
- Lewi L, Jani J, Blickstein I, Huber A, Gucciardo L, Van Mieghem T, et al. (2008). The outcome of monochorionic diamniotic twin gestations in the era of invasive fetal therapy: a prospective cohort study. American Journal of Obstetrics and Gynecology. 199(5):514.e1-514.e8.
- Wohlmuth C, Gardiner HM. (2022). Twin-twin transfusion syndrome: don’t rely on fluids and bladders to catch it early. Ultrasound in Obstetrics and Gynecology. 59(1):7–10.
 Abstract
Abstract  PDF
PDF